Positioning Isn’t Just for Wheelchair Use
It’s happened again. You’ve fitted your client for the perfect positioning wheelchair. They use it every day, but somehow, you’re still not seeing any lasting improvements. At this point, many physicians, therapists, or Assistive Technology Professionals (ATPs) could begin asking themselves how the wheelchair has failed. Many clinicians don’t consider that they can only achieve the desired results by maintaining correct patient positioning 24/7 – both in and out of the wheelchair.
Let’s consider the facts. Even if an individual uses their positioning wheelchair optimally for the majority of the day, other factors can have negative effects on the body. Often, strain from other parts of the everyday routine, such as sleeping, toileting, and transferring can outweigh the positive impacts of the positioning wheelchair. Despite consistent use of the proper tools, many patients experience negative outcomes. Proactive caregivers can avoid these negative outcomes by paying attention to positioning in other periods of the day or activities of daily living (ADLs).1 In order to get the most out of each custom positioning wheelchair, you must accommodate proper bodily position every hour of every day.
Consequences of Neglecting 24-Hour Positioning
If you rely solely on a positioning wheelchair to provide your patient’s posture support, then you leave them at risk for developing the following conditions.
Postural Deviations
As a person ages, their risk for postural deformities increases substantially.2 There are several factors that can lead to altered posture in an aging body, such as senile kyphosis (hardening of the intervertebral disks), osteopenia and osteoporosis (loss of bone density), sarcopenia (loss and of muscle).3 If correct bodily position isn’t maintained, then the person can develop deformities that can affect their mobility.
Loss of Mobility
Unquestionably, deformities can negatively impact the person’s ability to function, even in a wheelchair.2 They may develop a limited ability to self-propel, not to mention a higher dependence on caregivers. Eventually, the individual may become so uncomfortable that they are unable to tolerate sitting for long periods of time. This can certainly take a high toll on a person’s quality of life.
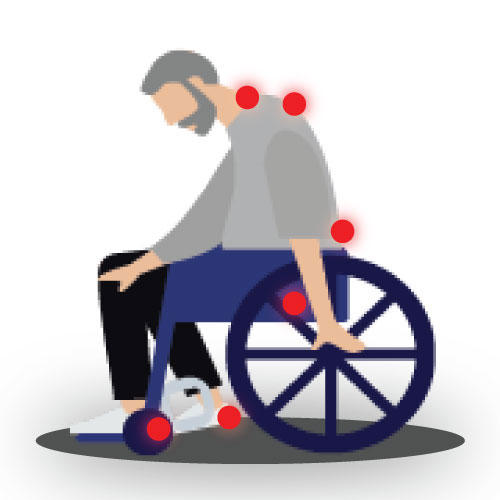 Pressure Injuries
Pressure Injuries
Incorrect positioning can also lead to inordinate amounts of pressure on bony prominences in the body. Due to this pressure, skin breakdown and pressure injuries can occur.4 In light of this risk, caregivers should be familiar with the most common places these wounds develop. Pressure injuries most often occur in the sacrum. In addition, common areas of concern include the heels, greater trochanter, ischial tuberosity, back of the head, ears, shoulders, elbows, inner knees, and malleoli.4 Be vigilant and check these areas frequently to catch a developing pressure injury in its earliest stages.
How to Adjust Positioning Outside of the Wheelchair
Postural Support in Bed
Outside of the wheelchair, a person with limited mobility will spend the largest portion of their day in bed. Musculoskeletal problems and pressure injuries can be prevented by paying attention to a person’s bodily alignment while lying down. There are many positioning aids that can be used in supine and lateral positions to maintain alignment of the person’s body.
 Correct bodily alignment consists of:
Correct bodily alignment consists of:
- Head facing up with eyes pointed straight ahead
- Neck straight
- Back straight
- Chest out
- Abdomen in
- Arms relaxed at the sides
- Knees slightly flexed
- Feet slightly apart with toes pointed forward5
If you notice the person’s body is not aligned appropriately, then you can use common household items as a positioning aid. For example, pillows provide soft support that can be rolled, folded, and tucked under the body. Additionally, towels, and wash cloths can be rolled to make forearm supports, hand rolls, trochanter rolls, and more.5 If the individual is completely immobile, then it’s important to change their position at least every two hours.5
Avoiding Pressure & Shear During ADLs
If a person is dependent on a caregiver for their ADLs, then they are more prone to pressure injuries.6 In this case, preventative measures can be taken during ADLs to avoid extra pressure and shear. Pay special attention to the strain placed on the skin during transfers and when dressing, toileting, and bathing, as these can be areas of risk for shear. Furthermore, you can treat pressure injuries with other measures, such as massage and nutritional arrangements.6
The Rewarding Results of 24-Hour Positioning Support
In summary, even if a person is properly positioned for 100% of the time spent in their wheelchair, that may not be sufficient for building and maintaining correct long-term posture and skin integrity. By paying attention to the key areas of pressure distribution, as well as contributing risk factors, caregivers can ensure that their patients are receiving the around-the-clock support they need to be healthy and get the most out of their positioning wheelchair.
Check Out Broda Positioning Wheelchairs
Need to upgrade your positioning wheelchair? Consider using a Broda positioning wheelchair for features such as endless adjustability and our proprietary pressure relief technology.
References
- Watanabe, L. (2021, August 1).24-hour follow through. Mobility Management. Retrieved October 19, 2021, fromhttps://mobilitymgmt.com/articles/2021/08/01/managing-posture.aspx?s=emob_090921&admgarea=emob&oly_enc_id=.
- Requejo, Philip S et al.(2015) Evidence-Based Strategies for Preserving Mobility for Elderly and Aging Manual Wheelchair Users. Topics in geriatric rehabilitation vol. 31,1: 26-41. doi:10.1097/TGR.0000000000000042
- Medical University of South Carolina. (n.d.).Posture change with age. What to Know: Posture Change with Age. Retrieved October 20, 2021, from https://muschealth.org/medical-services/geriatrics-and-aging/healthy-aging/posture.
- AlAboud, AM, Manna, B. (2021, July 1) Wound Pressure Injury Management. StatPearls [Internet]. StatPearls Publishing; 2021 Jan-. Retrieved October 20, 2021, from https://www.ncbi.nlm.nih.gov/books/NBK532897
- Stankovic, G. (2007, May).Positioning Techniques in Long-Term Care: Self-Directed Learning Package for Health Care Providers. Registered Nurses’ Association of Ontario
- Akbuğa,Gökçen & Mucuk, Salime. (2015). The Evaluation of Daily Living Activities, Pressure Sores and Risk Factors. Rehabilitation nursing: the official journal of the Association of Rehabilitation Nurses. 40. 10.1002/rnj.145.